AI-based Fall Detection and Pressure Ulcer Monitoring System for Long-term Care Facility Residents: The Feasibility Study
© 2025 by the Korean Physical Therapy Science
Abstract
This study aims to build a fall detection and pressure ulcer monitoring system that utilizes CCTV-based artificial intelligence (AI) technology specialized for nursing home environments to proactively detect and prevent falls and pressure ulcers in long-term care facility residents.
Feasibility study
This study focuses on the development a fall detection and pressure ulcer monitoring system utilizing observational data on the movements of residents in long-term care facilities, recorded through home-based CCTV. The observational data participants of this study were 26 patients with an average age of 83.8 years residing in a nursing home. Data were collected after obtaining written consent from the study participants or their legal representatives. Behavioral observation data will be collected for one hour per day for 20 days, taking into account participants' mealtimes, personal care, personal schedules, and sleep patterns. To assess the association between individual movement patterns and risk of falls and pressure ulcers, we assessed participants' general characteristics, risk of falls, risk of pressure ulcers, and cognitive function. This study develops a YOLO-Pose–based model that predicts key musculoskeletal points and detects related motion patterns from CCTV of long-term care facility residents. To train and test the system, motion data will be collected for different fall-risk scenarios, including partial upper-body movements or partial lower-body movements when getting out of the bed and attempts to lower the bed guard.
This study suggests the potential for developing an early fall detection and pressure ulcer monitoring system by integrating existing risk factors and real-time CCTV data in long-term care facility residents.
Keywords:
dataset, fall, motion, pressure ulcerⅠ. Introduction
Aging is rapidly progressing worldwide, and is recognized as one of the most significant demographic shifts facing humanity. According to a United Nations report, by 2050, over 30% of the population in 64 countries will be aged 65 and over, with significant implications across all sectors of society, including healthcare, welfare, the labor market, and the economy(de la Concepcion et al., 2017). South Korea is expected to enter a super-aged society (over 20% of the population aged 65 and over) by 2025, a rate much faster than that of advanced economies (Statistics Korea, 2023). In particular, with the baby boomer generation rapidly entering the elderly population, the proportion of the population aged 65 and over is expected to continue increasing over the next 20 to 30 years (Statistics Korea, 2024).
Aging does not simply mean a quantitative increase in the population, but also entails various complex problems directly related to the health, safety, independence, and quality of life of the elderly. Rapid aging is causing various social and medical problems, such as an increase in chronic diseases, dementia and cognitive decline, social isolation, a shortage of nursing staff and facilities, and a surge in medical and social security costs.(Montero-Odasso et al., 2022). These changes are significantly increasing the demand for senior care services, and the need for social welfare infrastructure, particularly long-term care facilities, is rapidly expanding (Kang & Kim, 2019). Consequently, systematic management and preventative measures to address key issues threatening the safety and health of seniors in long-term care facilities are becoming increasingly important.
Falls are one of the most common and dangerous accidents for older adults, and can have particularly devastating consequences for high-risk individuals with reduced physical function, such as those living in long-term care facilities (Ambrose & Hausdorff, 2013; Cameron et al., 2018). According to the Centers for Disease Control and Prevention (CDC), approximately 28% of the U.S. population aged 65 and older falls at least once per year (Grossman et al., 2018). Similarly, in Korea, approximately 25% of older adults aged 65 and older fall annually (Hwang et al., 2017).The incidence of falls, particularly among older adults admitted to long-term care facilities, is significantly higher than that of the general elderly population. This is recognized as a serious problem, not simply a matter of frequency, but one that impacts life, autonomy, and even social costs (Cameron et al., 2018). The most common physical injuries are fractures and traumatic brain injury. Fractures, if not properly treated and rehabilitated, can significantly impair the ability to perform daily activities. Traumatic brain injury can lead to cognitive decline or serious neurological damage (Verma et al., 2016).These physical injuries can lead to psychosocial problems, and the "fear of falling" that develops after a fall can lead older adults to limit their movements, leading to a reduced range of activities. This creates a vicious cycle that increases the risk of re-falling (Denkinger et al., 2015). This can exacerbate depression and feelings of helplessness, and in the long term, can even lead to social isolation.
Pressure ulcers are one of the health problems that frequently occur in elderly people residing in long-term care facilities with limited activity (Bak et al., 2008). When the same posture is maintained for a long time, the skin and soft tissues are continuously compressed, which blocks blood flow, leading to problems such as tissue necrosis, pain, infection, and delayed wound healing (Kim et al., 2011). Pressure ulcers are not just simple skin damage; they harm overall health and seriously reduce quality of life. In particular, in long-term care facilities, it is often difficult to regularly change patient positions or provide pressure ulcer prevention nursing due to lack of staff and limitations in care. As a result, pressure ulcers are often discovered late (Vanderwee et al., 2009).
Thus, fall and pressure ulcer are not simply accidents; they act as a complex risk factor that accelerates functional decline, significantly reduces quality of life, and increases social and economic burden (Painter et al., 2012). Therefore, it is crucial to establish a system that can prevent falls in advance and, when they occur, quickly detect and respond appropriately.In particular, in environments requiring constant care, such as nursing facilities, the number of residents is insufficient compared to the number of staff, and considering the difficulty in responding immediately to accidents at night or in blind spots, the introduction of a real-time fall detection system is essential (Ministry of Health and Welfare, 2022).
Early fall detection systems typically required users to press a button to request assistance. Later, wearable devices based on accelerometers or gyroscopes, pressure sensors, and bed/chair sensors were introduced (El-Bendary et al., 2013; De Miguel et al., 2017; Baec et al., 2015; Tanwar et al., 2022; Comai et al., 2024). However, these methods have several limitations, including resistance to wearing sensors, failure to detect when the device is not worn, difficulty distinguishing between daily activities and falls, and difficulty in maintenance(Alharbi et al., 2023, Mohan et al., 2024).
The CCTV-based artificial intelligence (AI) fall detection system is designed to analyze the movements of the elderly in real time by utilizing the CCTV infrastructure installed in existing nursing facilities, and automatically detect and warn of fall situations through a deep learning-based AI algorithm (De Miguel et al., 2017; Islam et al., 2020). Existing fall monitoring systems are often costly to construct and implement, and they primarily focus on detecting incidents after a fall has occurred(Tanwar et al., 2022). Moreover, these systems capable of simultaneously detecting both falls and pressure ulcers are rare(Silva et al., 2021). In contrast, this study proposes a low-cost system that not only enables fall detection and pressure ulcer prevention but also identifies early risk signs of falls through AI-based image analysis, providing preemptive warnings before an accident occurs. Recent advances in deep learning have made it possible to effectively distinguish between activities of daily living (ADL) and fall-related behaviors commercially viable, and various models are being applied to fall detection. CCTV-based AI systems offer privacy protection through a non-contact method, while also boasting high real-time performance, ease of installation, and cost-effectiveness. These systems could be ideal for use in confined environments like nursing homes, making them a next-generation fall prevention technology. Furthermore, systems could be built that automatically detect changes in the movement of older adults, analyze prolonged postures to predict the risk of developing pressure ulcer, and automatically provide alerts when there is a period of inactivity (Gruenerbel et al., 2023; Silva et al., 2021).
Therefore, this study aims to build a fall detection and pressure ulcer monitoring system that utilizes CCTV-based artificial intelligence (AI) technology specialized for long-term care facility environments to detect signs of fall risk in nursing home residents in advance to prevent falls, analyze whether they maintain posture for long periods of time to predict the possibility of developing pressure ulcers, and comprehensively prevent and manage secondary health problems that may arise.
Ⅱ. Methods
1. Participants
The sample size required for this study was calculated using G*Power Version 3.1.9.7 (Franz Faul, University Kiel, Germany, 2020) through statistical evaluation. For correlation analysis (one-tail, correlation p H1: 0.5, α error: 0.05, power: 0.8), a total of 23 participants were determined. Considering a dropout rate of 10–15%, 26 participants will be recruited. After obtaining approval for research participation and posting of recruitment notice from Gyeonggi-do G Nursing Home, data will be collected through movement observation of a total of 26 elderly people recruited through the recruitment notice. After the guardians of the research subjects receive a sufficient explanation of the research process from the research director, written consent for the research process will be obtained.
Eligibility criteria for study participants included residents of G Nursing Home, a long-term care certification level, and a Huhn's Fall Risk Scale score of 5 or higher, indicating a fall risk. Exclusion criteria included those with a Huhn's Fall Risk Scale score of 4 or lower, indicating no risk of falling, and those who did not obtain written consent from a guardian.
2. Method
This study focuses on the development a fall detection and pressure ulcer monitoring system utilizing observational data on the movements of residents in long-term care facilities, recorded through home-based CCTV. Observational data will be collected after obtaining written consent from the research subject or their legal representative for participation in the study. Behavioral observation data will be collected for one hour per day for 20 days, taking into account participants' mealtimes, personal care, personal schedules, and sleep patterns.
Prior to the experiment, this study will assess the general characteristics of the subjects, including gender, age, height, and weight. Furthermore, to understand the participant' physical and cognitive characteristics, fall risk, pressure ulcer risk, and cognitive function will be assessed.
Fall risk is measured using the Huhn Fall Risk Assessment Tool. This tool calculates a score from 0 to 24 based on eight items: the subject's age, mental status, bowel function, previous falls, activity level, walking and balance ability, and medication use. This score allows assessment of fall risk (low risk, initiate fall prevention measures, high risk, and very high risk), and in a neurological rehabilitation, this tool demonstrated a sensitivity of 98% for identifying fall risk(Hermann et al., 2018).
Pressure ulcer risk is measured using the Braden Scale, which consists of six items: sensory perception, moisture, activity, mobility, nutritional status, friction, and shear. Scores range from 6 to 23, and the assessment score for each item comprehensively identifies the risk of developing pressure ulcers (9 points or less - highest risk group, 10-12 points - high risk group, 13-14 points - intermediate risk group, 15-18 points - low risk group)(Wei et al., 2020). Interrater reliability expressed by the intraclass correlation coefficient ranged from 0.73 (95% CI 0.26–0.91) to 0.95 (95% CI 0.87–0.98)(Huang & Ma., 2021).
The Mini-Mental State Examination-Korean version (MMSE-K) will be used to assess cognitive function. The MMSE-K consists of 19 items, including orientation, memory registration, attention and calculation, memory recall, language, and visuospatial organization. Scores range from 0 to 30, with a score of 23 or lower considered cognitively impaired(Baek et al.,2016). MMSE-K shows moderate reliability (r=0.75)(Yang et al.,2002).
This study develops a YOLO-Pose–based model that predicts key musculoskeletal points and detects related motion patterns from CCTV of long-term care facility residents. To train and test the system, motion data will be collected for different fall-risk scenarios, including partial upper-body movements or partial lower-body movements when gettingout of the bed and attempts to lower the bed guard.
Using participants’ movement data collected from home CCTV, we constructed training, validation, and test datasets by extracting frames from video recordings and storing labeled information on participant’ movements and spatial ranges, which define their actions and positions and serve as essential input for accurate motion estimation and model training(Figure 1).
Predicting participants' falls and pressure ulcers through analysis of postural changes based on 21 key points.
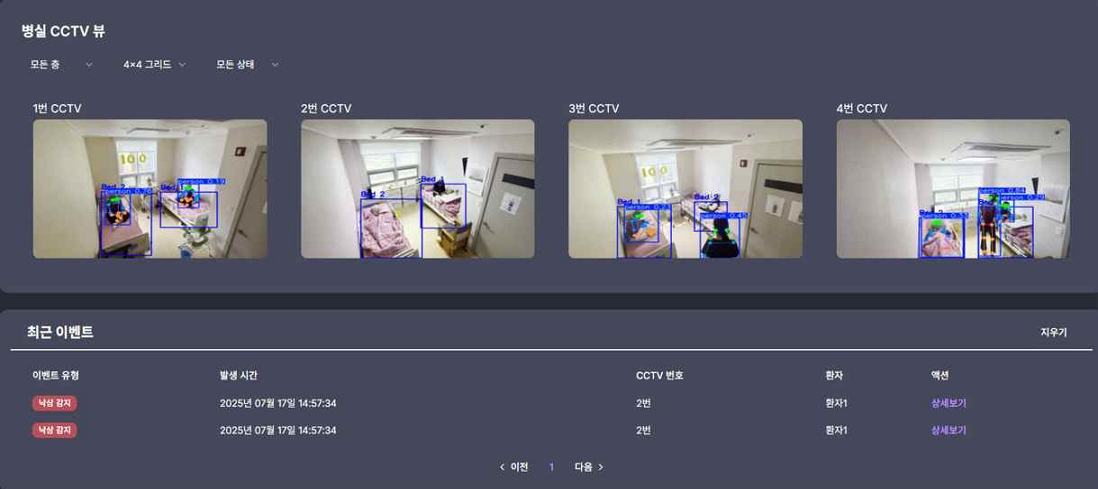
For fall detection, fall detection is performed based on head and hip keypoints, and the condition is determined as head Y coordinate > hip Y coordinate + 50 pixels, and only keypoints above 0.5 are valid, and false positives are reduced by distinguishing between normal posture changes and risky behaviors that cause falls.When a fall risk is detected, a "fall risk" event is automatically created and stored in the database with detailed information such as the occurrence time, location, patient information, and screenshots. Duplicate events are prevented with a 1-minute cooldown, and the event is automatically linked to the patient information assigned to the bed to accurately identify the patient and distinguish between fall risks inside and outside the bed area.
When pressure ulcer risk is detected, up to 120 frames (2 hours worth) of pose data are stored in a deque, and a mean absolute error of 0.1 or less is considered the same posture. Maintaining the same posture for more than 2 hours detects pressure ulcer risk, and continuous monitoring is implemented using a sliding window method.When a pressure ulcer risk is detected, a "pressure ulcer" event is automatically generated. Patient information, position duration, and risk level are stored in the database, with a one-hour cooldown to prevent duplicate events. Accurate patient identification is achieved by automatically linking to bed-assigned patient information, and the pose history is automatically reset after a risk event occurs.
To analyze and monitor the movements of long-term care facility residents, the extracted musculoskeletal key point data is utilized with a PC-based application software program, and the system is implemented with CCTV streams, an AI server (fall/pressure ulcer detection), a FastAPI backend, MongoDB/S3 storage, and a front-end dashboard(Figure 2).
3. Data Analysis
The camera software for data collection in this study will be developed using home CCTV, while data preprocessing software and deep learning–based computer vision models will be implemented in Python 3.10 with the PyTorch 2.3.1 framework. Statistical hypothesis testing will be conducted with SPSS version 27.0, including calculations of mean and standard deviation, and descriptive statistics will be applied to analyze the general characteristics of the study participants. The models will be compared using evaluation metrics such as mean Average Precision (mAP) and Intersection over Union (IoU) at a threshold of 0.5. Performance differences will be assessed with a custom-built validation dataset, and statistical significance between models will be tested using a t-test. To evaluate the intra-rater and inter-rater reliability of motion recognition results obtained from home cameras, the Intra-Class Correlation (ICC) will be calculated. A significance level of α = 0.05 will be applied for all statistical analyses.
Ⅲ. Discussion
This study aims to evaluate the feasibility of developing a deep learning–based computer vision model for predicting musculoskeletal key points and recognizing motions of residents in long-term care facilities using home CCTV. The study seeks to construct a learning dataset, design a training and inference pipeline, and develop a motion estimation system to validate the proposed approaches
Residents of long-term care facilities are typically older adults including the neurologic diseases and therefore at high risk of falls and pressure ulcers(Miura T. et al., 2025). Nevertheless, unexpected risks may also arise during the provision of care. While most existing fall detection systems focus on detecting falls after they occur, this study will focus on detecting falls in advance by analyzing the specialized movements of residents of long-term care facilities. Additionally, this study investigates development a specialized fall detection and bedsore prevention system by analyzing the underlying diseases and movement patterns of long-term care facility residents based on real-time CCTV recordings. The goal is to achieve a fall detection accuracy of over 70% and a pressure ulcer risk detection rate of over 90% in a real-world long-term care facility living environment, while developing an optimal algorithm that considers diverse environmental conditions and individual resident characteristics. This algorithm ensures stable detection performance even under diverse environmental conditions, such as lighting changes, shadows, and reflections. It also automatically responds to environmental changes with an adaptive threshold adjustment algorithm. Furthermore, it compares each resident's existing postural patterns to provide personalized analysis that detects fall and pressure ulcer risks. Additional performance analysis will be performed to optimize and streamline the model and verify the effectiveness of the developed fall risk detection and pressure ulcer monitoring system.
Ⅳ. Conclusion
This study aims to build a comprehensive dataset of residents in long-term care facilities, rather than relying on existing elderly fall data. It will develop a robust human posture estimation model that can cope with various environmental changes within the facility and subsequently create an AI-based fall and pressure ulcer risk monitoring system. By analyzing real-time CCTV data and preemptive risk factor data, we can track normal movement and provide valuable information to residents to anticipate risks in various movements and respond appropriately. This approach could save lives and reduce national care costs by supporting early fall detection, pressure ulcer prevention, and activity monitoring in long-term care facility residents.
Acknowledgments
This research was supported by the MSIT (Ministry of Science, ICT), Korea, under the National Program for Excellence in SW, supervised by the IITP (Institute for Information Communications Technology Planning & Evaluation) in 2025(2021-0-01440).
References
- 강성호, 김혜란. 노인장기요양서비스 현황과 보험회사의 역할 제고 방향. 보험연구원 연구보고서. 2019;2019(11):1-160.
- 이윤경, 이선희, 강은나, 김세진, 남궁은하, 최유정(2023). "2022년 장기요양실태조사 연구보고서." 보건복지부.
- 양동원, 조비룡, 최진영, 김상윤, 김범생. Korean Dementia Screening Questionnaire (KDSQ) 의 개발과 타당도 및 신뢰도의 평가. J Korean Neurol Assoc. 2002;20(2):000-.
- 통계청 (2023). "장래인구추계.“ https://www.kostat.go.kr/board.es?mid=a10301010000&bid=207&act=view&list_no=428476, “
- 통계청 (2024). "고령자통계." https://kostat.go.kr/board.es?mid=a10301010000&bid=10820&act=view&list_no=432917
-
Alharbi HA, Alharbi KK, Hassan CAU. Enhancing elderly fall detection through IoT-enabled smart flooring and AI for independent living sustainability. Sustainability. 2023;15(22):15695.
[https://doi.org/10.3390/su152215695]

-
Ambrose AF, Paul G, Hausdorff JM. Risk factors for falls among older adults: a review of the literature. Maturitas. 2013;75(1):51-61.
[https://doi.org/10.1016/j.maturitas.2013.02.009]

-
Baec S-H, Jeon M-S, Ko B-J. Implementation of Movement Detection System for Patient on Bed. Journal of Advanced Navigation Technology. 2015;19(5):458-63.
[https://doi.org/10.12673/jant.2015.19.5.458]

-
Baek MJ, Kim K, Park YH, Kim S. The validity and reliability of the mini-mental state examination-2 for detecting mild cognitive impairment and Alzheimer’s disease in a Korean population. PloS one. 2016;11(9):e0163792.
[https://doi.org/10.1371/journal.pone.0163792]

- Bak J, Gwon J, Lee J, Gang Ik LY, Kim D. Long term care insurance in elderly subjects and expansion study. Seoul: National Health Insurance Corporation. 2008:140-1.
-
Cameron ID, Dyer SM, Panagoda CE, Murray GR, Hill KD, Cumming RG, et al. Interventions for preventing falls in older people in care facilities and hospitals. Cochrane database of systematic reviews. 2018(9).
[https://doi.org/10.1002/14651858.CD005465.pub4]

-
Comai S, Lambruschi M, Ravasio F, Masciadri A, Pomante L, Salice F, editors. Enhancing Bed Safety: Monitoring Sleeping Positions, Bed-Exits, and Falls Using Grid-EYE Infrared Array Sensors. International Conference on Ubiquitous Computing and Ambient Intelligence; 2024: Springer
[https://doi.org/10.1007/978-3-031-77571-0_40]

-
de la Concepcion MAA, Morillo LMS, García JAÁ, Gonzalez-Abril L. Mobile activity recognition and fall detection system for elderly people using Ameva algorithm. Pervasive and Mobile Computing. 2017;34:3-13.
[https://doi.org/10.1016/j.pmcj.2016.05.002]

-
De Miguel K, Brunete A, Hernando M, Gambao E. Home camera-based fall detection system for the elderly. Sensors. 2017;17(12):2864.
[https://doi.org/10.3390/s17122864]

-
Denkinger MD, Lukas A, Nikolaus T, Hauer K. Factors associated with fear of falling and associated activity restriction in community-dwelling older adults: a systematic review. The American Journal of Geriatric Psychiatry. 2015;23(1):72-86.
[https://doi.org/10.1016/j.jagp.2014.03.002]

-
El-Bendary N, Tan Q, Pivot FC, Lam A. Fall detection and prevention for the elderly: A review of trends and challenges. International Journal on Smart Sensing and Intelligent Systems. 2013;6(3):1230.
[https://doi.org/10.21307/ijssis-2017-588]

-
Grossman DC, Curry SJ, Owens DK, Barry MJ, Caughey AB, Davidson KW, et al. Interventions to prevent falls in community-dwelling older adults: US preventive services task force recommendation statement. Jama. 2018;319(16):1696-704.
[https://doi.org/10.1001/jama.2018.3097]

-
Gruenerbel L, Heinrich F, Böhlhoff-Martin J, Röper L, Machens H-G, Gruenerbel A, et al. Wearable prophylaxis tool for AI-driven identification of early warning patterns of pressure ulcers. Bioengineering. 2023;10(10):1125.
[https://doi.org/10.3390/bioengineering10101125]

-
Hermann O, Schmidt SB, Boltzmann M, Rollnik JD. Comparison of fall prediction by the Hessisch Oldendorf Fall Risk Scale and the Fall Risk Scale by Huhn in neurological rehabilitation: an observational study. Clinical rehabilitation. 2018;32(5):671-8.
[https://doi.org/10.1177/0269215517741666]

-
Huang C, Ma Y, Wang C, Jiang M, Yuet Foon L, Lv L, et al. Predictive validity of the Braden scale for pressure injury risk assessment in adults: a systematic review and meta‐analysis. Nursing open. 2021;8(5):2194-207.
[https://doi.org/10.1002/nop2.792]

-
Hwang YS, Oh BT, Lee JY, Park SK, Hong SW, Kim DH, et al. Factors related with fear of falling in the Korean elderly. Korean Journal of Family Practice. 2017;7(5):640-5.
[https://doi.org/10.21215/kjfp.2017.7.5.640]

-
Islam MM, Tayan O, Islam MR, Islam MS, Nooruddin S, Kabir MN, et al. Deep learning based systems developed for fall detection: A review. IEEE Access. 2020;8:166117-37.
[https://doi.org/10.1109/ACCESS.2020.3021943]

-
Kim DH, Jeong HS, Lee DW. Evaluation of risk for pressure ulcers using the Braden Scale in elderly patients receiving long-term care. Journal of the Korean Geriatrics Society. 2011;15(4):191-9.
[https://doi.org/10.4235/jkgs.2011.15.4.191]

-
Miura T, Kanoya Y, editors. Fall Risk Assessment and Prevention Strategies in Nursing Homes: A Narrative Review. Healthcare; 2025.
[https://doi.org/10.3390/healthcare13040357]

-
Mohan D, Al-Hamid DZ, Chong PHJ, Sudheera KLK, Gutierrez J, Chan HC, et al. Artificial intelligence and iot in elderly fall prevention: A review. IEEE Sensors Journal. 2024;24(4):4181-98.
[https://doi.org/10.1109/JSEN.2023.3344605]

- Montero-Odasso M, Van Der Velde N, Martin FC, Petrovic M, Tan MP, Ryg J, et al. World guidelines for falls prevention and management for older adults: a global initiative. Age and ageing. 2022;51(9):afac205.
-
Painter JA, Allison L, Dhingra P, Daughtery J, Cogdill K, Trujillo LG. Fear of falling and its relationship with anxiety, depression, and activity engagement among community-dwelling older adults. The American Journal of Occupational Therapy. 2012;66(2):169-76.
[https://doi.org/10.5014/ajot.2012.002535]

-
Silva A, Metrôlho J, Ribeiro F, Fidalgo F, Santos O, Dionisio R. A review of intelligent sensor-based systems for pressure ulcer prevention. Computers. 2021;11(1):6.
[https://doi.org/10.3390/computers11010006]

-
Tanwar R, Nandal N, Zamani M, Manaf AA, editors. Pathway of trends and technologies in fall detection: a systematic review. Healthcare; 2022: MDPI.
[https://doi.org/10.3390/healthcare10010172]

-
Verma SK, Willetts JL, Corns HL, Marucci-Wellman HR, Lombardi DA, Courtney TK. Falls and fall-related injuries among community-dwelling adults in the United States. PLoS one. 2016;11(3):e0150939.
[https://doi.org/10.1371/journal.pone.0150939]

-
Vanderwee K, Grypdonck M, Bacquer DD, Defloor T. The identification of older nursing home residents vulnerable for deterioration of grade 1 pressure ulcers. Journal of clinical nursing. 2009;18(21):3050-8.
[https://doi.org/10.1111/j.1365-2702.2009.02860.x]

-
Wei M, Wu L, Chen Y, Fu Q, Chen W, Yang D. Predictive validity of the Braden scale for pressure ulcer risk in critical care: a meta‐analysis. Nursing in critical care. 2020;25(3):165-70.
[https://doi.org/10.1111/nicc.12500]